Date Posted, by Susan Jenks
We are posting this article in May for Hepatitis Awareness Month.
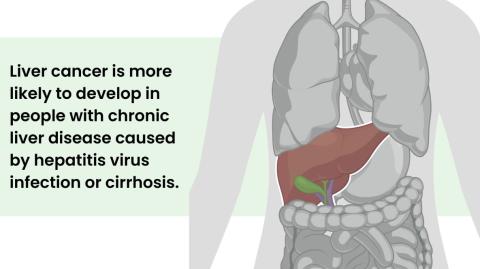
Despite intense research, liver cancer prevention remains a challenge, experts say, with efforts directed at underlying conditions that can significantly raise an individual’s risk.

“Liver cancer is unique in that 95% of those affected have underlying liver disease,” said Anna Suk-Fong Lok, M.D., Director of Clinical Hepatology and Assistant Dean for Clinical Research at the University of Michigan. “The best way to prevent liver cancer is to prevent liver disease from occurring in the first place.”
Moreover, she said, “You can’t go on only one risk factor,” in assessing an individual’s risk for liver cancer, given that many factors often contribute to its development. Although chronic infections with hepatitis B or hepatitis C viruses pose the leading threat, other risk factors include alcohol use, diabetes, obesity, cirrhosis, and scarring of the liver from any cause.
According to NCI data, an estimated 41,210 men and women in the U.S. will be diagnosed with liver cancer in 2023, and it’s estimated that nearly 30,000 individuals will die of these cancers this year—roughly double the number of deaths reported in 1980. Liver cancer is often detected late, with a poor 5-year survival rate of 19%. Finding the cancer at an early stage improves survival, but the 5-year survival rate of early-stage disease is just 37%, and recurrence of liver cancer remains a risk.
Liver transplantation can cure liver cancer and underlying liver disease, said Jo Ann Rinaudo, Ph.D., a program director in the Cancer Biomarkers Research Group in the National Cancer Institute’s Division of Cancer Prevention. However, “in patients who do not undergo transplantation, sometimes patients can develop a second liver cancer,” she said.
Therefore, preventing underlying disease from occurring is key to liver cancer prevention.
The Prevention Potential in Eliminating Hepatitis C
One recent effort in this direction is a proposed 5-year White House program to eliminate the most common viral risk factor for liver failure and liver cancers in the U.S., hepatitis C. The plan, part of the Biden-Harris administration’s fiscal year 2024 budget proposal, drew the support of the former director of the National Institutes of Health, Francis Collins, M.D., Ph.D., earlier this year in a commentary he co-wrote for the Journal of the American Medical Association.
In an interview accompanying the article, Dr. Collins, who is now a special advisor to President Biden for special projects, described the “dramatic and bizarre paradox” of hepatitis C, which causes a potentially curable blood-borne disease, yet still kills more than 15,000 people each year.
About 40% of those chronically infected with hepatitis C are not aware of their infections, Dr. Collins said, although they would benefit from receiving the blood test that identifies infection, as well as from treatments that have a 95% cure rate. Both the Centers for Disease Control and Prevention and the U.S. Preventive Services Task Force have recommended universal hepatitis C screening for all adults. “It seems like a public health success story that should have already happened,” Dr. Collins said in the interview. The fact that it hasn’t happened, he suggested, reflects several issues, including the hurdles people in marginalized communities often face in accessing screening and treatment.
Scientists have identified five hepatitis viruses. A vaccine exists to prevent chronic hepatitis B infection, and the CDC recommends that vaccine for all infants—given the high likelihood of transmitting infection between mother and child during pregnancy—as well as for all children and adolescents younger than age 19 who have not been vaccinated, all adults aged 19 to 59, and adults aged 60 or older with risk factors for infection. However, no vaccine yet exists for hepatitis C.
Hepatitis B and hepatitis C are considered different diseases. Hepatitis B poses more of a global threat, impacting an estimated 296 million people worldwide, according to data from the World Health Organization, while hepatitis C is more prevalent in the U.S., Europe, and Japan than in other countries. An estimated 2.4 million Americans are currently living with chronic hepatitis C infections.

Not only has that prevalence in the U.S. not budged in the last decade, “alarmingly, the incidence of new hepatitis C cases has, in fact, climbed, partly fueled by the opioid epidemic,” said T. Jake Liang, M.D., NIH Distinguished Investigator and chief of the Liver Diseases Branch in the National Institute of Diabetes and Digestive and Kidney Diseases. Even when treatment of the infection is successful, he said, patients can be re-infected with hepatitis C, illustrating the need for an effective vaccine to completely eradicate the disease.
In fact, Dr. Liang suggested that by 2040, projected deaths globally from hepatitis B and C together, if left unchecked, will outpace those due to HIV, malaria, and tuberculosis combined.
Vaccine efforts against hepatitis C have proven difficult due to greater sequencing divergence in hepatitis C compared with hepatitis B, HIV, or other human viruses, according to Dr. Liang. At least six major genotypes of hepatitis C have been identified worldwide, he said, and many more subtypes exist. “The ideal [scenario] will be if we can develop a vaccine that offers cross-protection against all of these [subtypes],” he said.
This is why identifying an effective hepatitis C vaccine is an active area of research. For example, in a recent NCI-supported phase 1 clinical trial, researchers studied the safety and immune response of a novel hepatitis C DNA vaccine administered alone or with an immune enhancer (interleukin-12). In their findings, published in the journal Cancer Prevention Research, the researchers reported that the dose with the immune enhancer was found to be safe and induced the strongest hepatitis C-specific immune responses. A phase 2 trial will study the vaccine’s antiviral effectiveness.
Targeting Other Underlying Disease
Ultimately, one strategy that might find more liver cancers in early-stage disease involves finding cirrhosis early, as well. Just as hepatitis viruses contribute to scarring and injuring the liver, so too does chronic alcoholism, or other forms of liver disease, such as nonalcoholic fatty liver disease. Therefore, screening for and treating cirrhosis are promising means of primary prevention for liver cancers, according to Amit Singal, M.D., Medical Director of the Liver Tumor Program and Chief of Hepatology at the University of Texas Southwestern Medical Center in Dallas. Over 90% of the most common type of liver cancers occur in the setting of cirrhosis, he said, accounting for an estimated 1-4% of these malignancies.
“We’re longing for some therapy to reverse cirrhosis, but there is none yet,” Dr. Rinaudo said. “If we can prevent cirrhosis from becoming a liver cancer, that would be a big win.”
If you would like to reproduce some or all of this content, see Reuse of NCI Information for guidance about copyright and permissions. Please credit the National Cancer Institute as the source and link directly to the blog post using the original title, for example: "Eliminating Underlying Liver Disease Remains Key Strategy for Liver Cancer Prevention was originally published by the National Cancer Institute." For questions, contact us at CancerPreventionBlog@mail.nih.gov.
