Project Title/Research Areas: Combined Breast MRI/Biomarker Strategies to Identify Agressive Biology
Principal Investigator/Institution: Victoria L. Seewaldt, MD, Duke University/Beckman Research Institute
Description of Current Activity
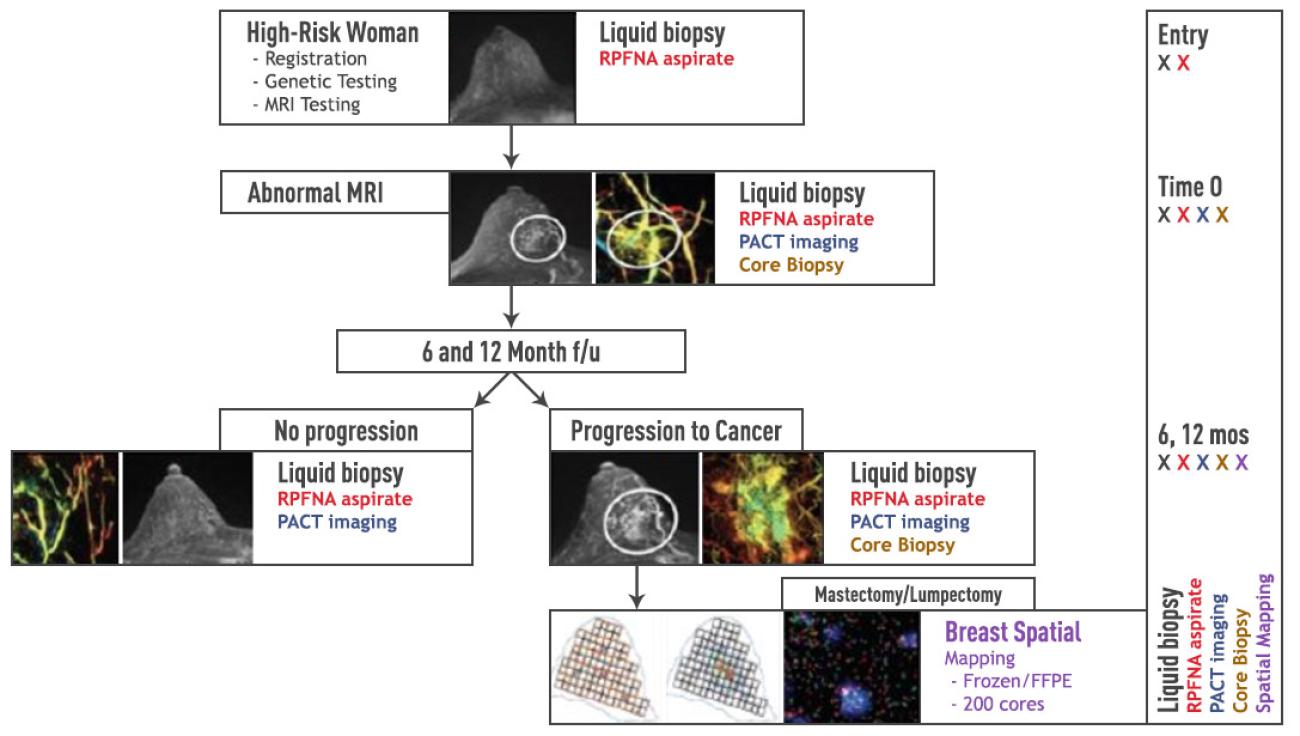
Breast Magnetic Resonance Imaging (MRI) has revolutionized high-risk breast cancer screening. However, while breast MRI is extremely sensitive, MRI has poor specificity. As a result, women are required to undergo frequent biopsy and expensive repeat MRI imaging. The vast majority of abnormal MRI and MRI-generated biopsies do not identify cancer, but still require extensive follow-up. This is because we are unable to determine whether a non-cancerous lesion identified by MRI has benign or aggressive biological potential. Here we are working to combine breast MRI and Wnt/p53-biomarkers to differentiate non-cancerous breast lesions with benign biology from those with aggressive biological potential. Our goal is to use combined breast MRI and p53/Wnt biomarkers to improve the specificity of MRI and reduce overdiagnosis and overscreening.
Currently, we are working to assemble, curate, and integrate imaging/biomarker studies performed at Duke University from 2005-2015. These studies provide serial imaging, tissue collection, and outcomes data from 300 women at high-risk for breast cancer. The cohort is highly annotated with genetic studies, menstrual data, progression data, medication data, serial BMI, and progression to cancer. Serial breast MRI, mammograms, ultrasound, and image guided biopsy have been de-identified. Whole exome sequencing has been performed on the WBC DNA from all 300 women. Serial biopsy samples are currently being sectioned and will be tested for: 1) gene expression, 2) proteomic profiling, and 3) targeted immunohistochemistry.
Our prospective MRI/biopsy/biomarker studies have recruited close to 100 high-risk women over a 6-month period. Many sites are just gearing up for recruitment, so it is anticipated that we will recruit over 500 high-risk women over the next 12 months.
Update
Retrospective Cohort:
We have downloaded, de-identified, and annotated, serial breast MRI imaging, mammograms, biopsies, and ultrasound imaging on 300 high-risk women. These women underwent prospective serial breast aspiration from 2005-2015. The corresponding WBC DNA and biopsy specimens have been identified. Genomic WBC DNA has undergone whole exome sequencing; biopsy specimens are currently undergoing immunohistochemistry analysis.
MRI's: total number: 1154- space needed: 1143GB
Mammograms: total number: 864- space needed: 86.4GB
Ultrasounds: total number: 225- space needed: 45GB
MRI biopsies: total number: 38- space needed: 7.6GB
Stereotactic (mammogram) biopsies: total number: 44- space needed: 8.8GB
Ultrasound biopsies: total number: 84- space needed: 8.4GB
Serial breast aspiration: 3,421
Breast biopsy specimens: 432
Prospective Cohort
Enrollment in our prospective MRI/biopsy cohort is underway. The trial is open at CoH and Duke. The trial has just opened at USC and Ohio State. U. Wisconsin is in the process of opening the trial. At CoH our trial opened 9/17. To date, we have enrolled 94 women over the past 6 months. We anticipate that recruitment will increase rapidly as other sites are up and running.